Among men who have sex with men (MSM), those living with HIV have a much higher syphilis diagnosis rate than those who are HIV negative. This disparity varies widely between states and could be driven in part by more frequent testing among HIV-positive MSM or minimized by more sexual contacts between the two groups.
Centers for Disease Control and Prevention (CDC) researchers presented their findings of a recent analysis of syphilis diagnosis rates among MSM in a poster presentation at the 2018 Conference on Retroviruses and Opportunistic Infections (CROI) in Boston.
Before conducting this analysis, which provided the first estimate of the ratio of syphilis diagnoses among MSM with HIV versus those without, the CDC researchers already knew that the majority of syphilis diagnoses between 2012 and 2016 were among MSM. During that period, between 48 percent and 57 percent of annual diagnoses among MSM were seen in those who had HIV.
The investigators looked at national case report data on syphilis diagnoses from 2014, which included for their purposes information on the sex of the person diagnosed, the sex of that person’s sex partner and the men’s HIV status. They limited their analysis to the 34 states that provided data that classified at least 70 percent of the syphilis cases as women, MSM or men who have sex with women only.
To develop a denominator for their analysis, the investigators relied on existing estimates of the size of the MSM population in each state.
Among all MSM, the syphilis diagnosis rate per 100,000 people across all 34 states was 237.7, ranging between 35.1 in Montana and 618.3 in Mississippi.
Overall, MSM living with diagnosed HIV had a syphilis diagnosis rate 7.8 times that of their HIV-negative counterparts: a respective 1,203 versus 155 per 100,000 MSM with and without HIV. The statewide syphilis diagnosis rate per 100,000 people among HIV-positive MSM ranged between zero in South Dakota and 2,035 in Arizona. Among HIV-negative MSM, the statewide syphilis diagnosis rate per 100,000 people in this group ranged between 27 in Montana and 496 in Mississippi.
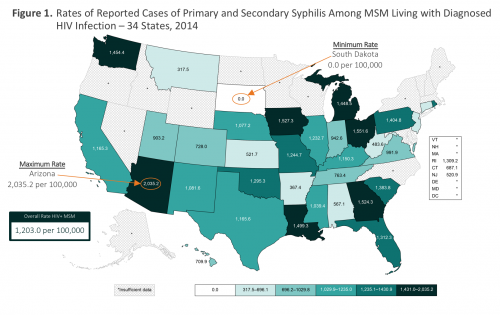
CDC, Grey et al, Estimated Primary & Secondary Syphilis Rates in MSM by HIV Status—34 States, 2014, CROI 2018 poster presentation

CDC, Grey et al, Estimated Primary & Secondary Syphilis Rates in MSM by HIV Status—34 States, 2014, CROI 2018 poster presentation

CDC, Grey et al, Estimated Primary & Secondary Syphilis Rates in MSM by HIV Status—34 States, 2014, CROI 2018 poster presentation
The ratio of HIV-positive versus HIV-negative syphilis diagnosis rates varied widely in each state (excluding South Dakota, the one state with no syphilis diagnoses). In Arkansas, HIV-positive MSM were 1.5 times more likely than their HIV-negative peers to receive a syphilis diagnosis, while this ratio was 21 in Utah.
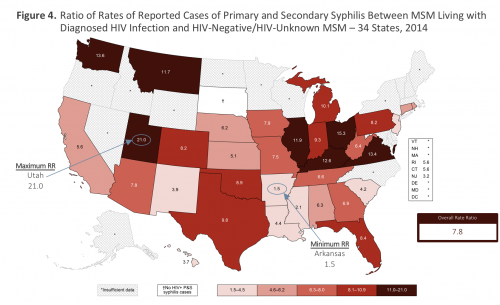
CDC, Grey et al, Estimated Primary & Secondary Syphilis Rates in MSM by HIV Status—34 States, 2014, CROI 2018 poster presentation
The CDC researchers speculate that the disparity in syphilis diagnosis rates may be driven in part by a greater rate of testing for the sexually transmitted infection among those MSM living with HIV compared with HIV-negative MSM. Additionally, they conjectured that in states with lower syphilis diagnosis ratios between MSM with and without the virus, more sexual interactions between these two groups might have spread the STI more evenly between them. The phenomenon of serosorting, in which MSM seek out sexual partners of their own HIV status, as well as differences in condom-use rates between those with and without HIV, might have increased the disparity.







Comments
Comments