In a move long encouraged by advocates, the World Health Organization (WHO) today reaffirmed that people living with HIV who consistently take antiretroviral treatment and have an undetectable viral load do not transmit the virus during sex, a concept known as Undetectable Equals Untransmittable, or U=U.
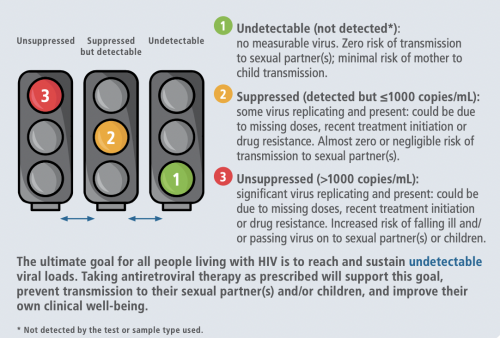
According to the WHO policy brief, released at the International AIDS Society Conference on HIV Science (#IAS2023) in Brisbane, Australia, people with an undetectable viral load who continue to take their medication as prescribed “have zero risk of transmitting HIV to their sexual partner(s)” and “minimal risk of transmitting HIV vertically to their children.” What’s more, people with a suppressed but detectable viral load “have almost zero or negligible risk” of sexual transmission. Data on the link between viral load and transmission via shared drug injection equipment are inadequate.
“I know that many in the HIV community will appreciate the clarity of this statement,” IAS president and conference cochair Sharon Lewin, MD, PhD, of the University of Melbourne, said at an advance media briefing.
World Health Organization
The WHO considers a viral load of 1,000 or less to be viral suppression, but the Centers for Disease Control and Prevention puts the threshold at 200 copies or less. A viral load below 50 is undetectable according to standard tests, though more sensitive tests can measure lower levels, and some assays used for research can measure down to a single copy.
The brief notes that a viral load test using a dried blood spot sample is as valid for determining viral suppression as a test that uses a plasma sample from a blood draw, making testing more accessible in more settings.
“The brief is a game changer for equitable scale-up of viral load testing and clear messaging about transmission risk,” Bruce Richman, executive director of the Prevention Access Campaign, told POZ. “This is the first time a global health institution has recommended that health care providers use and reinforce ‘zero risk’ to communicate U=U. There’s no room for ambiguity with ‘zero’!”
The brief “fills a gap in guidance on risk for folks with detectable viral loads between 200 and 1,000,” he added. “When the WHO’s new brief is translated from policy to implementation, millions more people living with HIV will have the assurance that their treatment is working to protect their health and their partners.”
The updated guidelines are supported by a systematic review of evidence published in The Lancet and presented at the conference by Lara Vojnov, PhD, of the WHO.

The Lancet
The review authors assessed evidence about sexual transmission of HIV linked to viral load in published studies and abstracts from 2010 to 2020 and other relevant data before 2010. They “found sexual HIV transmission to be absent” in cases involving a viral load less than 600 copies and “exceedingly rare” when viral load is below 1,000, Linda-Gail Bekker, MD, PhD, of the University of Cape Town, and colleagues wrote in an accompanying comment.
Vojnov and colleagues identified eight relevant studies with a total of 7,762 serodiscordant couples, mostly male/female. In three studies, there was no transmission when the HIV-positive partner had a viral load below 200. In four other prospective studies, there were 323 cases of HIV transmission, none of which occurred when partners with HIV were on stable suppressive antiretroviral treatment. Across all studies, there were two cases of transmission when the HIV-positive partner might have had a viral load below 1,000, but these are difficult to interpret due to the timing of viral load tests. Most transmission occurred when the HIV-positive partner had a high viral load above 10,000.
“There is almost zero risk of sexual transmission of HIV with viral loads of less than 1,000 copies per mL,” the study authors concluded. “These data provide a powerful opportunity to destigmatize HIV and promote adherence to [antiretroviral therapy] through dissemination of this positive public health message.”
Expanding Testing and Treatment
The WHO guidance also confirms that HIV-positive people who are diagnosed and treated early and take their medications as prescribed have improved health and life expectancy comparable to that of their HIV-negative peers.
A recent study in The Lancet HIV showed that people who are on treatment and maintain a high CD4 T-cell count can expect to live nearly as long as HIV-negative people in the general population. Early treatment initiation and good adherence can keep CD4s from falling into the danger zone for opportunistic illnesses and other health problems.
“For more than 20 years, countries all over the world have relied on WHO’s evidence-based guidelines to prevent, test for and treat HIV infection,” WHO director-general Tedros Adhanom Ghebreyesus, PhD, said in a statement. “The new guidelines we are publishing today will help countries to use powerful tools that have the potential to transform the lives of millions of people living with or at risk of HIV.”
According to a recent UNAIDS report released ahead of the conference, 29.8 million (76%) of the estimated 39 million people living with HIV worldwide are on antiretroviral treatment, up from 7.7 million in 2010. Of these, 71% have viral suppression. But this still leaves about 9 million people untreated and therefore at ongoing risk for disease progression and viral transmission. But children with HIV are not faring as well, with 57% on treatment and less than half with viral suppression.
In an effort to increase the number of people who know their HIV status and have access to treatment, the WHO’s new recommendations on HIV testing call on countries to expand the use of self-testing and to promote testing through sexual and social networks, especially in high-burden settings and regions with the greatest gaps in testing coverage. HIV self-testing may also be used by people who wish to start or continue pre-exposure prophylaxis (PrEP).
In the wake of changes in health care delivery brought about by the COVID-19 pandemic, “self-care and self-testing are increasingly being recognized as ways to increase access, efficiency, effectiveness and acceptability of health care across many different disease areas, including HIV,” according to the WHO.
In addition, a new WHO policy framework on primary health care and HIV aims to help decision-makers optimize work and collaboration to advance primary health care and response to diseases including HIV.
“Ending AIDS is impossible without optimizing opportunities across and within health systems, including with communities and in the context of primary health care,” said Jérôme Salomon, MD, MPH, PhD, WHO assistant director-general for universal health coverage, communicable and noncommunicable diseases.
Editor’s note: This article has been updated to clarify the meaning of “viral suppression” and “undetectable” and to add details from The Lancet paper and add a photo from IAS 2023.
Click here for more news about HIV treatment.
Click here for more reports from IAS 2023.







Comments
Comments