Much of our understanding of bone health has happened through research in postmenopausal women and older adults. The main concern for most people in these situations is to prevent bone loss and treat and perhaps reverse it once it’s happened. Two terms are used to describe bone loss: osteopenia and osteoporosis.
However, people living with HIV also experience bone loss, even at younger ages that these other groups. Research continues to look at the causes of osteopenia and osteoporosis in HIV-positive people and the ways in which to slow (or reverse) their progression.
What is bone?
Bone is living tissue that is in constant change over your lifetime. It’s made of several materials, mainly collagen and minerals. Collagen makes your bones flexible. Minerals, like calcium and phosphorus, help make it strong. Vitamin D is also important, as it helps the body absorb calcium and slows the kidneys from removing it.
To keep bones healthy, your body removes old bone tissue (bone resorption) with cells called osteoclasts as it adds new bone tissue (bone formation) with cells called osteoblasts. After that, bone density naturally declines over time because new tissue usually does not keep pace with bone loss. Therefore, as people age, bone tissue becomes less dense, weaker and more prone to injury. Other factors can contribute to it as well, such as poor nutrition, lack of activity, lower levels of sex hormones, and taking medications over time.
Who is at risk for bone loss?
Simply put, everyone, but these factors can contribute to it.
- Age—the older you are, the higher the risk.
- Sex—women face bone loss more often than men, though older men are at higher risk.
- Race—Caucasians and Asians are more likely to face bone loss. However, African Americans and Latinos are also at risk.
- Lifestyle—several things contribute to bone loss: smoking, alcohol use, excess caffeine, and inactivity.
- Diet—not eating the right type or amount of foods that have calcium or vitamin D raises your risk.
- Body size—in general, the smaller your bones and the thinner you are, the more at risk you are.
- Menopause—this is a risk factor for all women, including those whose periods stop before menopause.
- Hormones—bone loss can be due to low levels of testosterone, common in men with HIV.
- Medicines—certain drugs have been shown to increase bone loss, especially some that treat chronic health conditions and HIV.
- HIV—HIV’s activity in the body appears to increase bone loss.
What is osteopenia?
Osteopenia is a milder loss of bone density, and over 18 million Americans have it. Having osteopenia doesn’t mean you’ll develop osteoporosis. In fact, most people do not. However, a diagnosis of osteopenia may be a small wakeup call to do something about it. It likely can be stopped and even reversed.
First, osteopenia may be due to having a natural lower bone density. Second, there are ways to improve your bone health, including increasing your intake of calcium and vitamin D and getting more exercise.
Generally osteopenia has no symptoms. The only way to know you have this condition is by getting a bone density test done. Although this bone loss is generally less severe, it still means the bone has weakened some and may be prone to fractures.
What is osteoporosis?
Osteoporosis (which means “porous bone”) is a loss of bone mass and is the most common bone disease. In this condition, holes (lacunas) develop in the bone because newly formed bone tissue cannot fill in the holes. As it progresses, this weaker bone structure can cause the bones to become fragile and, as a result, increase the risk of fractures.
Over 10 million Americans live with it, and 3 out of 4 of them are women. It causes over 1.5 million bone fractures each year, mostly in the joints, spine, hips and wrists.
Primary osteoporosis is the natural loss of bone at any age, but it’s much more common in women after menopause and in men later in life. Secondary osteoporosis occurs from taking medicines or having a chronic condition. This may be more of an issue for people with HIV because of chronic illness, weight loss, medication use, etc.
Many men don’t think they’re at risk for osteopenia or osteoporosis. In general, men have larger frames and their bodies start losing bone later in life and at a slower rate. However, they’re still at risk, especially men with low levels of testosterone. Many men with HIV have low testosterone and may want to talk to their doctors about their bone health.
Symptoms of osteoporosis may not appear before a fracture happens. If they do, they may include joint pain and tenderness, backache, feeling of weakness and loss of height. After a fracture, the pain may be much more severe. The only way to know you have this condition is to get tested for it. Dental x-rays sometimes show bone loss, which may mean osteoporosis has occurred in other body parts.
How is it diagnosed?
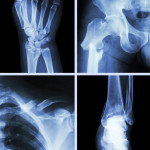
Bone mineral density (BMD) tests are the only way to detect osteoporosis. These tests are painless and noninvasive, and several tests area available: central machines that measure BMD in the hip, wrist, spine, or total body; and peripheral machines that measure it in the finger, hand, forearm, heel, or shin bone.
The most widely used and best understood test is called DEXA, or Dual Energy X-ray Absorptiometry. DEXA measures BMD of the spine, hip, or total body, and can detect as little as 2% of bone loss per year. DEXA uses about a tenth of the radiation of a chest x-ray. To conduct this test, the patient rests on a padded table. A large mechanical arm moves over the body, with a total body scan taking about 20 minutes to complete.
The result of a BMD test is given as a “T-score” or “Z-score”. Both measure “standard deviation,” or how far something is away from what is considered “normal.” The T-score compares women and men to a “normal” typically younger, healthy person of their own sex. A normal T-score is a number above -1.0. A score for osteopenia will be between -1.0 and -2.5, while osteoporosis is less than -2.5. The Z-score compares your BMD to someone of your own age, sex, weight and ethnic origin.
Currently, there are competing views on when to screen for bone problems in people with HIV. A 2009 set of recommendations by the Infectious Diseases Society of America suggests screening HIV-positive men and women who are over 50, but only if they have another risk factor. A more recent set of recommendations suggests that all HIV-positive men and women over 50 should receive bone scans.
What is the connection between HIV and osteoporosis?
Osteopenia and osteoporosis are more common among HIV-positive people, compared to HIV-negative individuals of the same sex and age. However, the reasons for this are not clear.
Is HIV infection itself to blame? Possibly. Various connections between HIV and bone loss are being studied. For example, HIV infection can increase certain proteins (IL-1, IL-6, TNF-a) in the body that may contribute to bone loss. It’s also possible that the constant immune inflammation caused by HIV may affect bone health. Some researchers have speculated that HIV-infected cells in the bone marrow may be to blame.
The use of HIV medications has also been linked to bone loss, which studies have described occur in various ways. Some meds may impair the way the body uses vitamin D. Some research suggests that mitochondrial damage can impair how osteoblasts function. Further, body shape changes have been linked to lower bone density.
Most studies show that using HIV meds typically results in a 2–6% bone loss within the first two years after starting treatment. This is about the same as that seen in women after the onset of menopause. Fortunately, longer-term use of HIV meds does not appear to cause progressive bone loss.
One thing is certain: the risk of osteopenia or osteoporosis increases with the length of time someone has been living with HIV. Moreover, HIV-positive people who have other risk factors for osteopenia or osteoporosis may be at higher risk for these bone problems.
What about prevention and treatment?
Although there is no cure for osteoporosis, there are ways to help prevent it and treat it. Almost 80% of your bone density is determined by heredity. The other 20% can be affected by changes in lifestyle. Currently, the ways to prevent bone loss in people with HIV are the same for postmenopausal women.
Calcium and vitamin D intake: Calcium plays an important role in maintaining bone health. Adults between 19 and 50 years of age should get 1,000 mg of calcium a day while those who are older should get 1,200 mg. However, surveys have shown that many Americans are not consuming enough calcium to maintain their bone health, including people living with HIV of all ages.
Foods rich in calcium include milk, cheese, tofu, broccoli and spinach. Other foods, including orange juice, can have calcium added to them by the manufacturer. Calcium supplements are also available through grocery stores, pharmacies, and health food shops. Discuss using any supplements with your doctor or pharmacist.
Vitamin D is also important, as it helps the small intestine to absorb calcium and slows the removal of calcium through the kidneys. Vitamin D is made in the skin after direct exposure to sunlight, and many people are able to get enough vitamin D with 30 minutes of sun a day. However, for other individuals, using vitamin D supplements is important. The major food sources of vitamin D are vitamin D-fortified dairy products, egg yolks, saltwater fish, and liver. Oral vitamin D tablets are also available, but high doses of vitamin D can also be harmful. Many vitamins and supplements already contain calcium and/or vitamin D.
Exercise: Both weight-bearing and resistance exercises are helpful. Being active day to day and exercising helps make bones denser and stronger, and weight-bearing activities force your body to work against gravity. These include power walking, jogging, climbing stairs, dancing or running, where your legs and feet support your body’s weight. Resistance exercises include stretching and lifting weights to help strengthen your muscles and bones.
Lifestyle changes: Maintaining a normal body mass index (when your body weight is proportional to your height and frame size) and avoiding tobacco and excessive alcohol use are key factors to consider.
Prescription drugs: Certain medications, especially if they are used at high doses or for long periods of time, can increase bone loss. For people who already are diagnosed with bone loss, stopping (or switching) certain drugs—including corticosteroids (prednisone, cortisone, etc.), phenobarbital, pentamidine, and ketoconazole—should be discussed with a health care provider.
It’s still not clear which HIV meds are most to blame for higher rates of bone loss. There are no recommendations about which should be avoided or switched. One particular drug—tenofovir DF (found in Atripla, Complera, Delstrigo, Stribild, Truvada and Viread)—increased bone loss on average 1–2% in clinical studies. However, no studies have found increases in fractures from its use. On the other hand, a newer version of tenofovir called TAF (Genvoya, Odefsey, Descovy) has shown less than 1% bone loss.
Antiresorptive Medications: Several prescription drugs approved by the FDA slow and possibly halt bone loss. It is important to note that most of them have only been studied in post-menopausal women experiencing significant bone loss or in older men with a secondary osteoporosis. Very little is known about how these agents affect women who are still menstruating or younger men. Even less is known about their use in HIV-positive people.
Antiresorptive medications are almost always used together with calcium and vitamin D supplements.
Bisphosphonates:
- Fosamax (alendronate): Alendronate is taken daily or weekly to prevent and treat postmenopausal osteoporosis. It is also approved for treating osteoporosis from long-term corticosteroid use in men and women. The drug also lowers the risk of spine, hip, and wrist fractures. Studies have shown that it is useful for increasing bone density in people living with HIV.
- Boniva (ibandronate): Ibandronate is a monthly tablet used to prevent and treat postmenopausal osteoporosis. It also reduces the risk of spine fractures, but no studies have been done in people with HIV.
- Actonel (risedronate): Risedronate can be taken daily or weekly to prevent and treat postmenopausal osteoporosis. It can also be taken by men and women to prevent and/or treat osteoporosis related to using corticosteroids. It lowers the risk of spine, hip and other fractures. No studies have been done in people with HIV.
Bisphosphonates are poorly absorbed. In turn, they must be taken on an empty stomach. All three drugs should be taken first thing in the morning. Alendronate and risedronate should be taken at least 30 minutes and ibandronate at least 60 minutes before eating or drinking anything other than water.
These medications can cause heartburn and erosion of the esophagus. It’s best to sit or stand for at least 30 to 60 minutes after taking them. They should not be taken immediately before bedtime.
These medications could theoretically cause jaw bone erosion and, paradoxically, weaker bones if taken over long periods. Thus far, studies of up to 10 years’ duration in HIV-negative women have shown extremely low rates of jaw problems and no additional fracture risk. Whether the same is true in people with HIV remains to be studied.
Hormone Therapy:
- Miacalcin (calcitonin): This hormone suppresses bone loss and slows the removal of calcium and phosphorous by the kidneys. It has only been approved for postmenopausal women with osteoporosis. It is not known if it is safe or effective for preventing or treating osteoporosis in HIV-positive men or premenopausal women.
- Estrogen: Synthetic estrogen is approved for preventing and treating osteoporosis in postmenopausal women. It is not used in men and is not recommended for premenopausal women. It is usually taken as a pill or given by a skin patch.
- Prempro: This daily pill contains both estrogen and progesterone, and reduces the risk of hip and other fractures. Possible side effects include risk of breast cancer, strokes, and heart attacks.
- Testosterone: This hormone is used in men only to slow or reverse decreased bone density and strength especially in the spine. Several brands come as an injection (taken every 2–3 weeks), a gel (rubbed on skin daily) or a skin patch. Many men report feeling better and having more energy, though it should not be taken by men with prostate cancer. Side effects can include swelling in the hands and feet and enlarged prostate gland and breasts.
Selective Estrogen Receptor Modulators (SERMs): These are a class of drugs that provide the benefits of estrogen therapy without its usual side effects. SERMs produce estrogen-like signals when they land on receptors of cells in the body, including osteoclasts. And because SERMs do not cause cells in certain tissues—such as breast and uterine tissue—to divide, the risk of breast and endometrial cancer using these drugs is reduced.
- Evista (raloxifene) is the only approved SERM to prevent and treat postmenopausal osteoporosis, increasing bone density at the neck and spine. It’s less likely to cause cancer of the uterus. Side effects can include hot flashes, leg cramps, blood clots, vaginal dryness, swelling, pain or tenderness, muscle and joint aches, and weight gain. It is not known if this drug helps to prevent or treat osteoporosis in premenopausal women with HIV.
Bone-Forming Medications: While bisphosphonates, hormone therapy, and SERMs have been shown to reduce bone resorption, one class of drugs has been shown to actually help build new bone.
- Parathyroid Hormone. Forteo (teriparatide), a form of this hormone, has been shown to increase bone density and strength in men and women. Parathyroid hormone helps your body store a healthy amount of calcium and phosphorus in your bones. Given by injection once a day, it’s currently only used for 24 months and costs more than other bone loss treatments. It is approved for treating osteoporosis in postmenopausal women. It is also approved to increase bone density in men with primary osteoporosis, or osteoporosis caused by low testosterone levels. Parathyroid hormone levels can be measured with a blood test. In postmenopausal women participating in clinical studies, teriparatide reduced the risk of fracture of the spine, hip, foot, ribs and wrist. In men, teriparatide reduced the risk of a spinal fracture.
Last Reviewed: September 14, 2018