Annual new HIV infections in the United States declined by 12% in recent years, according to the latest HIV surveillance report from the Centers for Disease Control and Prevention (CDC), released May 23. Increased use of pre-exposure prophylaxis (PrEP) played a role in this decline. While not everyone benefitted equally, all groups saw some improvement.
The CDC estimates that HIV incidence fell from about 36,500 new infections in 2017 to about 32,100 in 2021. But at this rate, “At least three people in the U.S. get HIV every hour—at a time when we have more effective prevention and treatment options than ever before,” according to Robyn Neblett Fanfair, MD, MPH, acting director of the CDC’s Division of HIV Prevention. About two thirds of people with new infections are gay or bisexual men, and more than half live in the South.

CDC
“We see some bright spots in the data—our nation’s HIV prevention efforts are working, especially for young people,” Jonathan Mermin, MD, MPH, director of the CDC’s National Center for HIV, Viral Hepatitis, STD, and TB Prevention, said during a media briefing this week. “While we are on the right track, progress is not happening quickly enough or equitably among all people or in all areas of the country. A challenging task that once seemed impossible—to end the HIV epidemic in America—is possible. We need the will, the resources and the resolve to make it happen.”
HIV Incidence
The CDC compiles new HIV diagnoses reported by local jurisdictions and also estimates HIV incidence, or the total number of new infections, both diagnosed and undiagnosed. According to the agency, 87% of the estimated 1.2 million people living with HIV have been tested and know their status. However, less than 60% of people ages 13 to 24 and only about 70% of those ages 25 to 34 have been diagnosed.

CDC
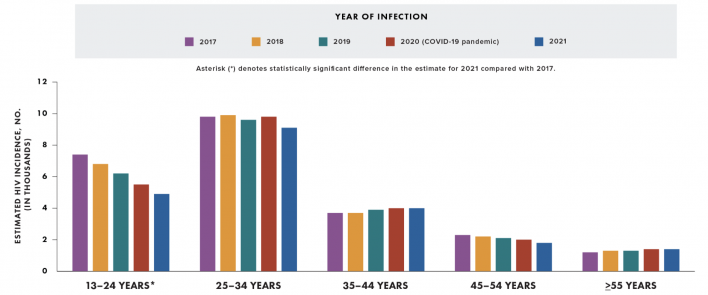
The decline in incidence was driven by a 34% drop among people ages 13 to 24, from about 9,300 new infections in 2017 to about 6,100 in 2021. This age group accounts for the second largest number of new infections, after people ages 25 to 34 (12,600). Young gay and bisexual men, who account for 80% of HIV cases in this age group, saw new infections fall from about 7,400 to about 4,900. But the decline was not even: Cases fell by 45%, 36% and 27% among young white, Latino and Black gay and bi men, respectively.
Just under 20% of new HIV infections in 2021 were among women, more than half of whom were Black. Overall, Black people make up about 12% of the U.S. population but account for 40% of new HIV cases. Latinos make up about 18% of the population and account for 29% of new cases.
Looking at HIV among infants, the surveillance report notes that the United States has met its goals for eliminating perinatal HIV, with the rate of mother-to-child transmission falling below 1% for the first time in 2019 and continuing to decline. As recently reported in the journal Pediatrics, the annual perinatal diagnosis rate declined from 1.9 cases per 100,000 live births in 2010 to 0.9 cases in 2019. The new report shows a further decline to 0.6 cases in 2021.

CDC
In 2021, the South saw more new infections (16,700) than the West (6,600), Midwest (4,400) and Northeast (4,400) combined. However, it was the only region to see a statistically significant decline, falling by 12%.
The CDC notes that numbers for 2020 and 2021 should be interpreted with caution due to disruptions in HIV testing and other services during the early years of the COVID-19 pandemic, but the decline in HIV incidence among men appears to be steady.
HIV Care
Turning to HIV care indicators, described in a separate report, more than 80% of people diagnosed with HIV were linked to care within a month after their diagnosis. The portion of diagnosed people who were on antiretroviral treatment with an undetectable viral load rose slightly, from 63% in 2017 to 66% in 2021. But here, too, not everyone benefitted equally. An estimated 72% of white people achieved viral suppression, compared with 64% of Latinos and 62% of Black people.
The drop in HIV incidence and the rise in the proportion of people on treatment in the United States pales in comparison with some other high-income countries, such as the United Kingdom and Australia. In the United Kingdom, efforts to reduce HIV among gay and bi men have been so successful that they now account for fewer new cases than heterosexuals. The differences can be attributed to “deeply entrenched social determinants of health that drive disparities and make progress elusive for many people in the United States,” Mermin said. “Health disparities will naturally occur in unequal society.”
The most successful countries have gotten more people with HIV on treatment, and people with viral suppression do not transmit the virus, a concept dubbed Undetectable Equals Untramsittable (U=U). According to Neblett Fanfair, people in the United States who receive care through the Ryan White HIV/AIDS program have outcomes rivaling those seen in more successful countries, showing that lack of health insurance and access to care is contributing to disparities.
The Role of PrEP
The nationwide decline in HIV incidence mirrors an increase in PrEP use. Among the 1.2 million people the CDC estimates could benefit from prevention pills or shots, about 30% had a prescription in 2021, up from 13% in 2017. But Black and Latino people are less likely to use PrEP even though they account for a majority of those at risk for HIV. According to the new report, 78% of white people at risk were taking PrEP in 2021, compared with 21% of Latinos and 11% of Black people. PrEP use also remains low among women, at around 12%.

CDC
President Joe Biden’s FY2024 budget proposal includes $850 million—a 48% increase over this year—to accelerate efforts to end the HIV epidemic. Biden has also proposed $237 million for a national PrEP program. But these requests may not be met, as some legislators have called for deep cuts in federal spending to balance the national budget.
“It appears that our investments in HIV prevention are providing some positive results, but the persistent high number of new diagnoses and the low usage of PrEP among the communities most impacted by HIV point to the need for increased resources, particularly for a national PrEP program,” Carl Schmid, executive director of the HIV+Hepatitis Policy Institute, said in a statement. “While there have been some increases, they have not been at the level needed to put the U.S. on a path to end HIV.”
The availability of generic versions of Truvada (tenofovir disoproxil fumarate/emtricitabine, or TDF/FTC) has helped increase PrEP access, Mermin noted. More people are now insured compared with 2017, thanks to the Affordable Care Act and Medicaid expansion during the pandemic. But these gains could be reversed now that the national COVID-19 public health emergency has ended. Likewise, mandatory insurance coverage of PrEP is also in jeopardy due to a Texas judge’s ruling in March that is currently on hold pending an appeal.
At the current rate, the country is not on track to meet the goals of the Ending the HIV Epidemic initiative, which calls for a 90% decrease in new infections and for 95% of people diagnosed with HIV to be on treatment with viral suppression by 2030.
To get there, CDC officials stress the need for increased investment in proven prevention programs, maximizing innovation—such as by expanding self-testing and use of long-acting injectable treatment and PrEP and by offering services in more settings—and centering equity to better reach people disproportionately affected by HIV.
“Our nation’s HIV prevention efforts continue to move in the right direction,” CDC director Rochelle Walensky, MD, MPH,
. “Longstanding factors, such as systemic inequities, social and economic marginalization and residential segregation, however, stand between highly effective HIV treatment and prevention and people who could benefit from them. Efforts must be accelerated and strengthened for progress to reach all groups faster and equitably.”
Click here for more news about Ending the HIV Epidemic.






Comments
Comments