After decades of research, a microbicidal gel—in this case made from the antiretroviral drug tenofovir—has finally proved effective in preventing transmission of HIV in women, cutting the overall infection rate by 39 percent. These data were reported Tuesday, July 20, at the XVIII International AIDS Conference in Vienna and were met with a prolonged standing ovation from delegates in attendance.
The results were also published online July 19 in the journal Science.
AIDS researchers have been seeking a biomedical HIV prevention tool since the virus was first isolated 27 years ago. During the past 15 years, given the poor progress being made on a vaccine, much attention has been focused on developing microbicidal gels. Unfortunately, 11 studies of six different products have so far failed to find an effective microbicide, and at least one study found that the microbicide being tested actually placed women at greater risk of contracting HIV.
 | |
| Result of CAPRISA 004 reviewed by Quarraisha Abdool Karim during a press conference at the XVIII International AIDS Conference in Vienna. |
Previous studies have reported that a 1 percent tenofovir gel was highly effective at reducing viral transmission in monkeys, either when used daily or intermittently. Small studies in humans found the gel generally safe and well tolerated. The first large study to explore the effectiveness of the gel in humans was the Centre for the AIDS Program of Research in South Africa (CAPRISA) 004 study, the results of which were reported today.
How the Study Worked
CAPRISA 004 enrolled 889 HIV-negative, sexually active women in two areas of South Africa: Durban, an urban center, and a rural area about 150 kilometers outside Durban. Previous preparatory studies found the rate of new HIV infections to be extremely high among women in both regions—about 6 percent of women became infected in the urban location each year, and 11 percent in the rural location.
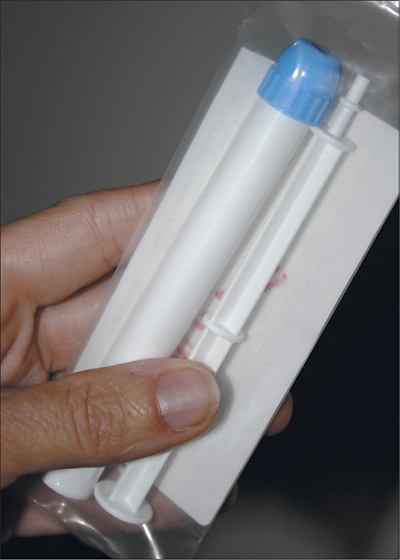
In the study, women received extensive safer-sex counseling and condoms. They also received single-dose pre-filled applicators that contained either the tenofovir gel or a placebo to use 12 hours before insertive intercourse and within 12 hours after. The women received detailed instructions regarding the proper use of the microbicide, and they received monthly counseling to support adherence throughout the study. Adherence was measured both by self-report and by the return of all used and unused applicator packs to the study sites.
The study’s results were reported at the International AIDS Conference and published in Science by a husband and wife team—Salim Abdool Karim, MD, and Quarraisha Abdool Karim, MD, from the Columbia University Mailman School of Public Health in New York City and CAPRISA in Durban—and their colleagues.
Promising Results
The authors found that the tenofovir gel far out-performed the placebo gel, and that the beneficial effect became evident early on.
During the 30 months of follow up, 98 women out of the 889 became HIV positive during the trial—with 38 in the tenofovir gel group and 60 in the placebo gel group. The HIV incidence was 5.6 percent in the tenofovir gel group and 9.1 percent in the placebo gel group.
 | |
| New findings indicate that an experimental microbicide helps reduce risk of HIV infection. |
It is worth noting that efficacy dwindled as the study continued. The tenofovir gel cut the HIV infection rate by more than 50 percent at the 12-month study mark, but dropped to 39 percent at the final 2.5-year study mark. This was likely due to adherence fatigue—less consistent use of the gel as time went on.
In women who remained highly adherent, defined as women who used the gel in more than 80 percent of their sex acts for all 30 months of the study, the drop in transmission remained high—54 percent. With average adherence or poor adherence, the reduction in new infections was 38 and 28 percent, respectively.
“Without this gel, for every 100 women we may see 10 women being infected in a year,” said Salim Abdool Karim, as reported by the U.S. Department of Health and Human Service’s website healthfinder.org. “With this gel, we would see only six women being infected.”
Out of the 434 women who tested negative for herpes at the start of the trial, 29 became infected in the tenofovir group and 58 became infected in the placebo group. This translated into a 51 percent reduction in the rate of genital herpes transmission.
The rate of side effects was similar between those receiving the tenofovir gel and those receiving the placebo gel, though the tenofovir gel users had higher rates of diarrhea. The authors stated that there is no known reason for such an effect. There were four cases of a hepatitis “flare” in women infected with hepatitis B virus (HBV)—a temporary worsening of symptoms of hepatitis-related liver problems—but the four cases were split evenly between those on tenofovir and those on placebo.
Researchers have been concerned that continued use of the gel, after a person becomes infected with HIV, might cause the development of tenofovir-resistant HIV to emerge. Fortunately, in this study, no tenofovir resistance was found in any of those who became infected while using the gel. The authors cautioned that further research will be needed to confirm these results. In fact, another study looking at daily tenofovir gel use is already in progress. It’s likely, however, that an even larger clinical trial might be needed before the gel can be approved and licensed around the world, said Kevin Fenton, MD, PhD, the director of the National Center for HIV/AIDS, Viral Hepatitis, STD and TB Prevention at the U.S. Centers for Disease Control and Prevention.
On a positive note, one of the great fears of prevention researchers—that women would compensate for a perceived reduction in HIV transmission risk from the gel and use condoms less frequently—did not occur. In fact, reported condom use actually rose during the course of the study.
In contrast, the authors stressed that adherence to the gel was low. “Despite [extensive adherence counseling and support] and high gel acceptability, about 40 percent of the women in this study had below 50 percent gel adherence. Future trials will need to place greater emphasis on enhancing and objectively measuring adherence, in light of its substantial influence on the trial outcome,” they said.
Ultimately, better packaging and a sexier marketing message could help increase adherence.
“This is simply a cylindrical white plastic tube. You can’t get anything more unattractive,” said Salim Abdool Karim. “Even Coke would have gone bankrupt if they had adopted this approach to their marketing. We only made this gel for the study. I think the future is going to involve making this gel sexy, making this gel something that is part-and-parcel of the sex act, that enhances sex. Packaging is part-and-parcel of addressing the adherence issue.”






5 Comments
5 Comments