More than half of the world’s HIV population is now on antiretroviral (ARV) treatment.
Michel Sidibé, executive director of the Joint United Nations Programme on HIV/AIDS (UNAIDS), made this once-unthinkable pronouncement at a July press conference in Paris’s storied Hôtel de Ville.
Specifically, an estimated 19.5 million out of 37.6 million people living with HIV are on ARVs. Meeting this benchmark—an accomplishment Sidibé touted as “extraordinary”—indicates that the global health community is making progress toward achieving the ambitious, if not audacious, targets for controlling the epidemic that UNAIDS set in 2014.

French AIDS ambassador Michèle Boccoz, executive director of UNAIDS Michel Sidibé, mayor of Paris Anne Hidalgo and Christine Kafando, a community health worker from Burkina Faso, speak at a press conference on the new 90-90-90 UNAIDS report.Benjamin Ryan
UNAIDS has pushed nations toward getting 90 percent of their respective HIV populations diagnosed, 90 percent of that group on ARVs and 90 percent of that group virally suppressed. According to the agency’s modeling, achieving these 90-90-90 targets by 2020 will set national epidemics on a path toward ending HIV as a major public health threat by 2030.
This concerted drive is geared around the powerful twofold benefit of HIV treatment: Not only do ARVs grant a near-normal life span, but they also prevent transmission when the virus is fully suppressed. In short: Successfully treating HIV impedes its global spread. At least in theory. Recently, some HIV researchers have grown impatient waiting for strong evidence that HIV’s powerful individual preventive effect has grand-scale results, significantly lowering overall infection rates. They are concerned that if an outsize proportion of HIV transmissions originate from those recently infected, then diagnosing and treating such individuals fast enough to break the chain of new infections may prove highly challenging.
According to UNAIDS’s new report on the global epidemic, the recent push to diagnose and successfully treat HIV in hard-hit nations has driven the 2016 global equivalent of the 90-90-90 target to an auspicious 70-77-82 (meaning that 70 percent of those living with HIV are diagnosed, 77 percent of that group is on ARVs and 82 percent of that group is virally suppressed). However, these figures are less impressive when considering that they signify that only 44 percent of the global HIV population is virally suppressed, a far cry from the 73 percent rate that hitting the 90-90-90 target would yield.
Nevertheless, encouraging signs of worldwide progress abound. Since 2010, the estimated annual rate of new infections among adults has declined 11 percent, from 1.9 million to 1.7 million, while the rate for children has plunged 47 percent, from 300,000 to 160,000. And since its peak in 2005, the AIDS-related death rate has fallen by nearly 50 percent, hitting 1 million last year.
A primary driver of these global trends has been the full-court press against the devastating epidemic in eastern and southern Africa, home to just over half of the world’s HIV population. Having hit 76-79-83 on its way to the 90-90-90 target and an overall viral suppression rate of 50 percent, the 19-nation region saw its rate of annual new infections drop 29 percent between 2010 and 2016 while its AIDS-related death rate fell by 42 percent.
HIV treatment as prevention appears to be working


At the Paris press conference, in reference to the 2014 launch of the 90-90-90 targets, an ebullient Sidibé said, “For most people at this time, it seemed impossible.” As for the present day, he said, “I’m proudest to say that we can be satisfied with our achievements. This just goes to show that the resources that we have devoted to our cause are starting to bear fruit.”
The resources are considerable, even as they remain troublingly inadequate. Total funding to combat HIV in low- and middle-income nations has remained flat for three years. Between 2015 and 2016, overall contributions from major wealthy donor nations to this effort slumped from $7.5 billion to $7 billion, their lowest level since 2010. Meanwhile, domestic funding from the nations receiving such aid has been on the rise, hitting 57 percent of the overall $19.1 billion spent in 2016. But such increases have slowed—and likely have their limits. According to UNAIDS, an extra $7 billion is needed annually for the total response in poorer nations. The agency is pushing for $26.2 billion by 2020, an annual ask that its number crunchers project will decline to $23.9 billion by 2030 as HIV is increasingly brought under control.
“Of course, we still need to do more,” Paris’s Mayor Anne Hidalgo stressed at the Hôtel de Ville press conference. “We need to continue to strive for an end to the epidemic. It is really a question of political will.”

Mayor of Paris Anne Hidalgo at the press conference for the release of the UNAIDS 2017 HIV epidemic progress report at Paris’s Hôtel de VilleBenjamin Ryan
*****
The release of the UNAIDS report supercharged the launch of the 9th International AIDS Society Conference on HIV Science in Paris (IAS 2017). More than 7,000 HIV researchers, clinicians and advocates met at the biennial confab to share research findings, celebrate successes and take stock of deficiencies in hopes of honing their methods.
The mammoth Palais des Congrès conference hall, which housed IAS 2017, boasts a central venue that, appropriately for the occasion, resembles a rock concert hall. In an age when celebrity is prized above all else and antiscience, anti-intellectual populist uprisings threaten nations’ capacity to reap the benefits of scientific inquiry, the endearingly geeky MDs, PhDs, MScs and the like who took to the stage throughout the conference proved themselves to be nothing if not rock stars in the global fight against HIV.
However, powerful countervailing winds threaten their efforts. Linda-Gail Bekker, MD, PhD, president of the International AIDS Society and the conference’s international scientific chairperson, addressed such concerns in no uncertain terms at the gathering’s opening session.
“Nationalistic forces are rocking this world,” a forceful Bekker said. “When I think over the past year, a word that comes to mind is chaos. It’s unsettling, and it’s frightening.”

Linda-Gail Bekker, PhD, the International AIDS Society (IAS) President and International Scientific Chair of IAS 2017 in ParisBenjamin Ryan
Like many of the conference’s presenters, Bekker was keenly aware that this event amounted to a cri de coeur to wealthy donor nations for desperately needed, huge financial commitments.
Referring to the United States, she said, “The largest and most important global donor in the HIV response has threatened devastating cuts to funding for research and treatment programs.” Then, addressing the overall funding retreat on the part of wealthy nations, she continued, “These onslaughts on funding, principles and programs have already begun to erode the gains we have so painstakingly made. If we are not actively moving forward on the HIV response, then we are sliding back. Sliding back means sick patients, lost lives, ongoing transmission and infected children.”
In May, President Donald Trump, in keeping with his America-first brand of hypernationalism, presented a budget proposal for the 2018 fiscal year that included a desired 17 percent cut (from $4.6 billion to $3.8 billion) in funding for the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) in poorer nations and a 19 percent cut (from $1.35 billion to $1.1 billion) to The Global Fund to Fight AIDS, Tuberculosis and Malaria. In addition, Trump sought to slash by 23 percent the budget for the National Institutes of Health (NIH), the scientific powerhouse that drives much of the world’s most vital HIV research.
In the days leading up to the conference, Sidibé tended toward a glass-half-full perspective on the global epidemic with a seasoned showman’s excited, staccato delivery. But he changed his tune after protesters stormed the stage at the opening session and highlighted a sobering reminder of the global shortcomings in combating HIV: the death from pneumonia of the revered South African HIV activist Prudence Mabele less than two weeks earlier. Slated to speak after the protest, Sidibé told the crowd of thousands that he was compelled to dispense with his prepared speech and then proceeded to get more real.

UNAIDS executive director Michel Sidibé, speaking from the heart at the opening session of the conference.Benjamin Ryan
“I want to say it will be dishonest to leave this podium without saying that we are failing,” Sidibé said. He noted uneven progress in the global HIV fight and, in particular, a failure to properly address the treatment needs of the nearly half million children living with the virus in west and central Africa who are still not receiving ARVs.
Joining Bekker in a call for increased global funding, he put the matter simply: “Like the French people say, maintenant ou jamais.”
Now or never.
*****
Arguably the most important player at the conference was Deborah L. Birx, MD, the Obama-appointed U.S. global AIDS coordinator and head of the PEPFAR effort. Cut from the same cloth as Mathilde Krim, the venerable amfAR founder whom she cited as a mentor, Birx boasted the regal glamour of a Camelot-era socialite with the wonkish expertise of a scientific Hillary Clinton. Serving as a tidy foil to the more boisterous and broad-strokes-focused Sidibé, Birx provided ongoing commentary about HIV surveillance statistics that was guided by the buzzword coloring the conference: granularity.
Don’t fall for “the tyranny of averages,” Birx cautioned conferencegoers. Looking only at top-line statistics about the epidemic, such as a national viral suppression rate, she stressed, can mask the urgent unmet needs of various subgroups.

Ambassador Deborah Birx, the US Global AIDS Coordinator and Director of PEPFAR at IAS 2017Benjamin Ryan
A granular, or highly precise, look at surveillance data can help better characterize and drive the response to the epidemic among key populations. KPs, as they are known, include men who have sex with men (MSM), transgender people, sex workers, injection drug users (IDUs) and the sexual partners of all such individuals. These groups make up 56 percent of global HIV cases, including 25 percent of the epidemic in sub-Saharan Africa and 80 percent in other regions across the globe.
“Unless you crack the problem with key populations, you’re never going to get the 90-90-90 implemented well,” Anthony S. Fauci, MD, director of the U.S. National Institute of Allergy and Infectious Diseases (NIAID, a division of the NIH), told POZ. “Because if you look at the key populations, they drive the epidemic.”
“The problem is that HIV is moralized, and therefore it is politicized,” said Solange Baptiste, the executive director of the International Treatment Preparedness Coalition (ITPC). “If we are honest, we know that governments will not prioritize those most affected by HIV.”

Anthony S. Fauci, MD, director of the National Institute of Allergy and Infectious Diseases (NIAID), speaking at IAS 2017Benjamin Ryan

Solange Baptiste, executive director of the International Treatment Preparedness CoalitionBenjamin Ryan
After taking the reins at PEPFAR in 2014, Birx directed her agency to better break down its surveillance data by factors such as sex, age, subregion and KP in order to better tailor local responses.
“I want to be very clear that we are constantly looking at where we are failing,” Birx said. “We are not as generous as UNAIDS in saying people have reached the 90-90-90 until all genders and all age bands have reached the 90-90-90.”
Such failures include the inefficient allocation of funds. For example, Birx said it has recently cost as much as $1,000 to find and diagnose one person living with HIV in certain parts of Africa, especially in remote regions. That’s more than the cost of a year of treatment.
Birx sounded a particularly loud alarm about the considerable failure to adequately diagnose and treat young people in eastern and southern Africa. She also warned that high fertility rates and recent successful efforts to prevent childhood mortality in the region mean that a “youth bulge” will likely soon drive up the numbers of adolescents and young adults with HIV as that sizable generation ages into sexual activity.
Overall global statistics can also mask worrisome trends in major regions. Eastern Europe and Central Asia, which UNAIDS categorizes as one region, is alone in experiencing a worsening HIV story. According to the agency’s report, the area that includes Russia and various former Soviet states has seen its annual HIV infection rate and AIDS-related death rate rise a respective 60 percent and 27 percent during the current decade. Only 28 percent of the region’s HIV population is on ARVs. Stigmatization and criminalization of gay sex and injection drug use are apparently major drivers of these trends.

The proportion of the HIV population that is on treatment in Eastern Europe and Central Asia has risen sluggishly while the rate of AIDS-related deaths continues to climb.UNAIDS
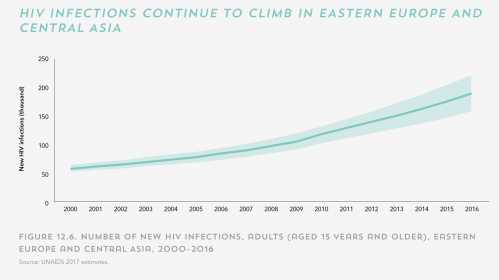
The rate of new transmissions of HIV in Eastern Europe and Central Asia has continued to climb while it has generally fallen elsewhere in the world.UNAIDS
Meanwhile, west and central Africa, home to 17 percent of the global HIV population, has made disappointing progress in combating the virus compared with the rest of sub-Saharan Africa. Hitting a target of only 42-83-73 and a viral suppression rate of just 25 percent, the region has experienced a relatively meager 9 percent decline in its HIV infection rate since 2010.
During the conference, a small team from AIDS Healthcare Foundation (AHF) provided skepticism about the reliability of the UNAIDS global estimates, going so far as to argue that the agency might have inflated figures for political gain. Jorge Saavedra, MD, MPH, global public health ambassador at AHF, challenged the conference speakers doggedly, generally painting a gloomier portrait of the epidemic.
“They use diplomacy,” Saavedra said of UNAIDS in an interview with POZ. “They want to highlight the gains, and they don’t mention the things that are not really working well.”

Jorge Saavedra, MD, MPH, global public health ambassador at AHF, peppered presenters with skeptical questions throughout the conference.Benjamin Ryan

AIDS Healthcare Foundation’s booth at the conference adhered to the organization’s tendency to highlight a glass-half-empty perspective on the epidemic.Benjamin Ryan
PEPFAR has been keen to address the critical need for more precise epidemic-tracking methods. The agency has driven the recent rollout of a revolutionary surveillance method known as a population-based HIV impact assessment, or PHIA, in an increasing number of African nations. Instead of relying on mathematical modeling based on limited data sets, PHIA estimates spawn from a large, nationally representative sample of household surveys—a far more reliable and rich source of information.
A recent PHIA study served as the foundation for one of the conference’s most exciting presentations. A beaming Velephi Okello, MD, deputy director of health services at the Swaziland Ministry of Health, announced that in five years, hard-hit Swaziland has doubled its national viral suppression rate, from 37 percent to 74 percent, while cutting its infection rate in half. These impressive results came on the heels of recent PHIA studies indicating that between 60 and 68 percent of the national adult HIV populations in Malawi, Zambia and Zimbabwe are virally suppressed.
“We are going to build upon these successes,” Okello said. “In the end, we would like to see a Swaziland that is free from AIDS.”

Current statistics about the progress to the UNAIDS goals to get 90% of national HIV populations diagnosed, 90% of that group on ARVs and 90% of that group virally suppressed by 2020—known as the 90-90-90 targets.PEPFAR

Velephi Okello, MDBenjamin Ryan
*****
Researchers made a case for increased resources to combat global HIV in economic terms as much as in humanitarian terms. Spend big now, save later is a guiding principle behind the 90-90-90 targets. Ramping up ARV treatment in the short term will prevent new infections and the costly need to treat even more people for the rest of their lives. Of course, this calculus could change if researchers develop successful treatments that can prompt extended viral remission and freedom from daily ARVs—a reality that may grace at least some people with HIV during the 2020s.
“In this day and age, we can’t afford to do things that don’t work, that are not really efficient and not helpful in controlling the epidemic,” Wafaa El-Sadr, MD, MPH, told POZ. She’s the director of the global health organization ICAP at Columbia University’s Mailman School of Public Health; PEPFAR funds ICAP to lead the PHIA studies.

Wafaa El-Sadr, MD, MPH, epidemiologist at Columbia University at IAS 2017Benjamin Ryan
A barrage of presentations analyzed the benefits of various approaches to improving the 90-90-90 figures. There was a strong emphasis on abandoning one-size-fits-all, clinic-based care in hard-hit nations in favor of differentiated care, a highly flexible HIV-care model that can be tailored to individual needs, perhaps relying on relatively inexpensive community health workers to help reach far-flung communities.
Other tactics discussed included using HIV self-testing kits, rolling out Truvada (tenofovir disoproxil fumarate/emtricitabine) as pre-exposure prophylaxis (PrEP), merging HIV health services with those addressing numerous other health issues, as well as promoting greater generic drug discounts and investing more heavily in the ARV supply chain to address the alarming frequency of drug stockouts in poorer nations.
Expanding viral load testing in such countries as a way to guide treatment decisions is likely crucial given the World Health Organization’s warning that in numerous surveyed nations more than 10 percent of those starting HIV treatment today have a strain of the virus that is resistant to some of the most widely used ARVs. Clinicians are hoping that expanded global use of the integrase inhibitor Tivicay (dolutegravir), a highly potent ARV with a high barrier to viral resistance, may help mitigate this looming threat.
So what about the cold hard cash? Questioned about the Trump administration’s proposed budget cuts to international HIV funding, a diplomatically sanguine Birx suggested that reason would prevail.

PEPFAR head Deborah L. Birx, MD. The photo at her waistband is of the recently departed South African HIV activist Prudence Mabele.Benjamin Ryan
“They understand this pandemic, and they understand what needs to be done and are deeply committed to changing the course of the pandemic forever,” Birx said of the president’s team. Noting that business people are at the helm of the federal government, Birx said she was more than prepared to speak to them in familiar terms: promising a proven return on investment.
“I think that sometimes we’re not used to making a good business case,” Birx said. That includes the failure to present estimates of what global HIV would look like had the United States never begun its HIV-related international-aid funding push during the 2000s.
Proposing an answer to that question, Jessica McGillen, MS, D.Phil, a research associate at Imperial College London, presented the findings of a modeling study that suggested that 4 million more people would have contracted HIV and an additional 5 million people would have died of AIDS-related causes in sub-Saharan Africa had the George W. Bush administration not started massively investing in this region, prompting greater contributions from wealthy nations and African countries in the process. And McGillen projected that if overall funds for international aid for HIV remain flat going forward, the proportion of people with HIV on successful ARV treatment in this region will likely stagnate accordingly.

Jessica McGillen, PhD, of Imperial College, LondonBenjamin Ryan

Jessica McGillen, PhD, presents a key slide that projects the impact of U.S. funding on viral suppression rates in 18 sub-Saharan African nations.Courtesy of Benjamin Ryan
Fortunately, according to numerous accounts, there is still strong bipartisan support in the U.S. Congress for continued, if not increased, funding for international HIV, as well as an actual boost in funding for the National Institutes of Health. But whether the conferencegoers’ calls for support from other wealthy donor nations, in particular the United Kingdom, the Netherlands, France and Germany, fell on receptive ears remains to be seen in this era of geopolitical instability.
In the meantime, after the dutiful graduate students rolled up the last of the poster presentations at the conclusion of IAS 2017, conference attendees took what they learned in Paris and fanned out across the globe. They returned to the halls of influence in Washington, DC, or to the laboratories of the world’s finest universities, or to the unpaved roads of African villages to continue their work.
They set out to save the world from the scourge of HIV. And given enough money and political will and, most important, scientific know-how, before long, they very well could succeed.

A Parisian ad campaign to fight the epidemic, featured in the Métro, evokes New York City’s “Play Sure” campaign with its sex-positive messaging: “Make Love.” Benjamin Ryan
Benjamin Ryan is POZ’s editor at large, responsible for HIV science reporting. His work has also appeared in The New York Times, New York, The Nation, The Atlantic and The Marshall Project. Follow him on Facebook, Twitter and on his website, benryan.net.










Comments
Comments